Introduction
Neuralgia refers to severe, stabbing, or shooting pain along a nerve pathway. It can occur due to various causes, including nerve damage, inflammation, or irritation. Neuralgia can be a chronic condition that significantly impacts daily life and requires proper management and treatment.
Symptoms
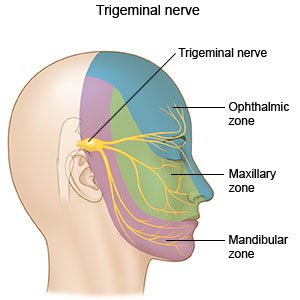
The primary symptom of neuralgia is intense, sharp, and shooting pain that follows the path of a specific nerve or nerves. The pain may come and go, but it can be triggered by certain activities, movements, or even by touch. Common types of neuralgia include trigeminal neuralgia (affecting the facial nerves), occipital neuralgia (involving the nerves in the scalp), and postherpetic neuralgia (resulting from nerve damage after a herpes zoster infection).
Diagnosis
Diagnosing neuralgia involves a thorough evaluation by healthcare professionals, such as neurologists or pain specialists. They will review your medical history, conduct a physical examination, and may order tests to rule out other potential causes of the pain. Imaging tests, such as MRI scans, may be performed to identify any structural abnormalities or nerve damage. In some cases, nerve conduction studies or diagnostic nerve blocks may be utilized to pinpoint the source of the pain.
Treatment
Treatment for neuralgia aims to alleviate pain and improve quality of life. The specific approach depends on the underlying cause and severity of the neuralgia. Treatment options may include:
Medications: Over-the-counter pain relievers, such as nonsteroidal anti-inflammatory drugs (NSAIDs), may be recommended for mild cases. For more severe or chronic neuralgia, prescription medications like anticonvulsants, tricyclic antidepressants, or muscle relaxants may be prescribed to help control pain signals and provide relief.
Nerve Blocks: Injecting a local anesthetic or steroid medication near the affected nerve can help temporarily block pain signals and provide relief. Nerve blocks can be performed under the guidance of imaging techniques, such as ultrasound or fluoroscopy.
Physical Therapy: In some cases, physical therapy may be beneficial for neuralgia. Therapeutic exercises, stretches, and techniques like transcutaneous electrical nerve stimulation (TENS) can help reduce pain and improve nerve function.
Surgical Interventions: If conservative treatments are ineffective, surgical interventions may be considered. Procedures such as nerve decompression, radiofrequency ablation, or neurectomy (surgical removal of a nerve) may be recommended in certain cases.
Lifestyle Changes
In addition to medical treatments, making certain lifestyle changes can help manage neuralgia:
Stress Management: Stress can exacerbate pain, so implementing stress-reduction techniques like relaxation exercises, meditation, or mindfulness can be helpful.
Heat or Cold Therapy: Applying heat or cold packs to the affected area may provide temporary relief and help reduce pain and inflammation.
Gentle Exercise: Engaging in low-impact exercises, such as walking, swimming, or yoga, can help improve overall well-being, reduce stress, and promote better pain management.
Avoiding Triggers: Identifying and avoiding triggers that worsen neuralgia symptoms is important. These triggers may include specific movements, activities, or environmental factors that exacerbate pain.
Good Sleep Habits: Maintaining a regular sleep schedule, ensuring a comfortable sleep environment, and practicing relaxation techniques before bed can improve sleep quality, which may have a positive impact on pain management.
Supportive Network: Building a support system of family, friends, or support groups can provide emotional support and help cope with the challenges of living with neuralgia.
Remember, neuralgia can be a complex condition, and finding the most effective treatment approach may require patience and collaboration with healthcare professionals. With the right combination of treatments, lifestyle adjustments, and support, individuals with neuralgia can better manage their pain and improve their quality of life.







